What Are Herxheimer Reactions?
Herxheimer reactions, also simply referred to as “Herx” reactions, are temporary exacerbations of symptoms that can occur shortly after starting a treatment for certain infections. Herxheimer reactions often occur when large numbers of pathogens are killed off rapidly by IV treatments, medications, supplements or other treatments like infrared sauna or hyperbaric chamber. When these pathogens die, they release toxins and other harmful substances into the body. The sudden release of toxins can overwhelm the kidney and liver’s ability to eliminate them, leading to an inflammatory response that manifests as a worsening of symptoms.
This die off can also be the patient’s own senescent (or zombie) cells. Cellular senescence is a state in which cells cease to divide and undergo functional changes, typically in response to stress or damage. This process is characterized by permanent cell cycle arrest and is associated with aging, tissue degeneration, and various diseases, including cancer. Various treatments can induce apoptosis (or cell death) in senescent cells and this often doesn’t feel good though it is a part of the healing process.
What symptoms manifest with Herxheimer reactions?
- Fever
- Chills
- Headache
- Muscle aches
- Joint pain
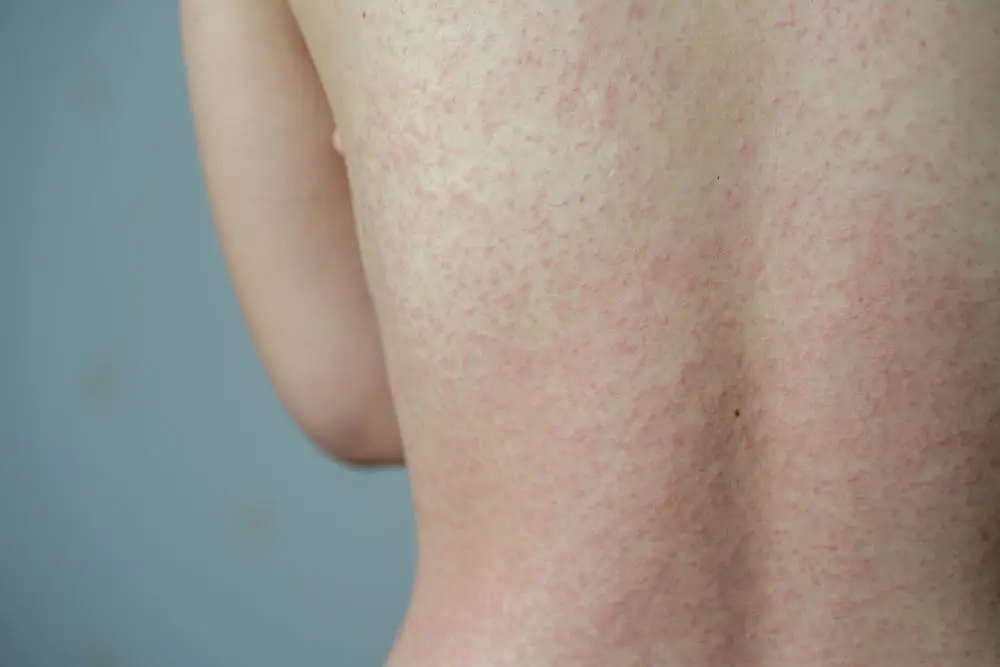
- Skin rashes/irritation
- Pressure
- Discomfort
- Body aches
What triggers a Herxheimer reaction?
A Herxheimer reaction can be elicited by any therapy that is causing the destruction of endotoxin-creating organisms or causing the release of endotoxins from places they are being stored in the body, such as:
- Ozone IV or insufflation
- High dose vitamin C
- Antibiotics
- Anti-parasitics
- Anti-virals
- Antimicrobials
- Any oxidative therapy that boosts immunity or kills pathogens
How can I support my body during a Herxheimer reaction?
- Listen to your body and rest! You may feel fatigued or may be experiencing aches and pains. Adjust your routine as necessary.
- Hydrate! Your body needs fluids in order to flush out toxins and the byproducts of immune processes and cell turnover, as well as to repair your cells. Focus on hydrating foods such as fruits and vegetables, fresh pressed juices, and spring water or filtered water with a pinch of sea salt or lemon juice.
- Sweat! If you body is able to, sweating through exercise or sauna allows for metabolic waste and toxins to be excreted through the skin. Make to sure to shower immediately after sweating before the concentrated sweat is reabsorbed back into the skin.
- Try a Ginger Detox Bath. It seems silly, but taking a hot bath full of goodies that help the body to release toxins is a great way to reduce the symptoms of a Herxheimer reaction. The night following a treatment, or whenever you feel your body may need aid in detoxifying.
How to do a ginger detox bath:
- 1/4 cup of fresh grated ginger or 1/2 teaspoon powdered ginger (from your local supermarket or health food store)
- 1 cup of Epsom salts
- 2 tbsp baking soda
- 1 cup white distilled vinegar
- 1/2 cup powdered ascorbic acid
- 1/2 cup himalayan pink sea salt crystals or Dead Sea salts
- An alternate option is using essential oils instead of ginger. Don’t use it at the same time. Add ten drops of essential oils of your liking (i.e. lavender for stress relief, peppermint or wintergreen for pain and nausea, clove and copaiba for muscle ache and inflammation).
- Make sure to stay hydrated and drink lots of water during this process.
Are Herxheimer reactions a positive sign of healing?
Yes it is a sign that your body is working the treatment. It does not mean the treatment is wrong necessarily but may mean you need to lower your dosage significantly and slow down the process to a rate you can tolerate. During this time, follow the recommendations above to aid the process and support the detoxification process.
Also read: Victoria Roberts At Meeting Point Health