How to Evaluate a Stem Cell Clinic: 6 Questions to Ask
Stem cell therapy is one of the most exciting frontiers in modern healthcare and regenerative medicine, but for the average patient, it is also one of the most overwhelming. Between conflicting terminology, varying cell sources, and the sheer complexity of cellular signaling, it is easy to feel lost. Choosing a stem cell provider shouldn’t feel like a high-stakes gamble; it should be a decision based on clinical transparency and medical rigor.
At Meeting Point Health, we believe that when a therapy is this complex, your provider’s knowledge is your greatest safety net. To help you move from confusion to clarity, here are the six essential questions you should ask to evaluate a clinic’s clinical standards.
1. What are the types of stem cells being used?
Not all stem cells are created equal. When evaluating a provider, it’s important to distinguish between autologous (cells harvested from your own bone marrow or fat) and allogeneic (cells donated from healthy, full-term birth tissues).
At Meeting Point Health, we choose allogeneic sources for several specific clinical reasons:
- The Age Factor: Your stem cells age as you do. Research shows that as we age, the number of Mesenchymal Stem Cells (MSCs) in our bone marrow declines, and the cells that remain become less robust and slower to multiply.
- The Biological Potential: Allogeneic cells from umbilical cord tissue are considered to be “biologically young.” They haven’t been exposed to decades of environmental toxins, oxidative stress, or chronic illnesses. These cells often have higher proliferative potential and a more powerful paracrine effect, the ability to signal your other cells to begin healing.
- Avoids Invasive Procedure Routes: Using allogeneic cells means you don’t have to undergo a painful bone marrow aspiration or liposuction procedure to harvest your own tissue. This aims to reduce overall treatment time, discomfort, and the risk of infection at the harvest site.
- Provides Consistency & Standardization: Autologous samples are highly variable from patient to patient. By using screened, allogeneic cells, we can ensure a standardized dose of high-viability cells that have been rigorously tested by third-party labs for safety and potency.
2. Who is performing the procedure, and what is their specific training?
Stem cell therapy is a highly technical medical intervention. You are not just paying for a product; you are paying for the clinical judgment and anatomical expertise of the person holding the needle. The training qualification you should look for is:
- Triple Board-Certification: At Meeting Point Health, procedures are performed by Dr. Matta, who is triple board-certified in Primary Care, Non-Surgical Orthopedics, and Stem Cell Therapy.
- Why it Matters: A triple board-certified physician understands how your systemic health (Primary Care) affects your musculoskeletal system (Orthopedics) and how to harness biological signals (Stem Cell Therapy) to bridge the two.
- The Non-Negotiable: Certification and extensive expertise are your greatest insurance policies for both safety and efficacy.
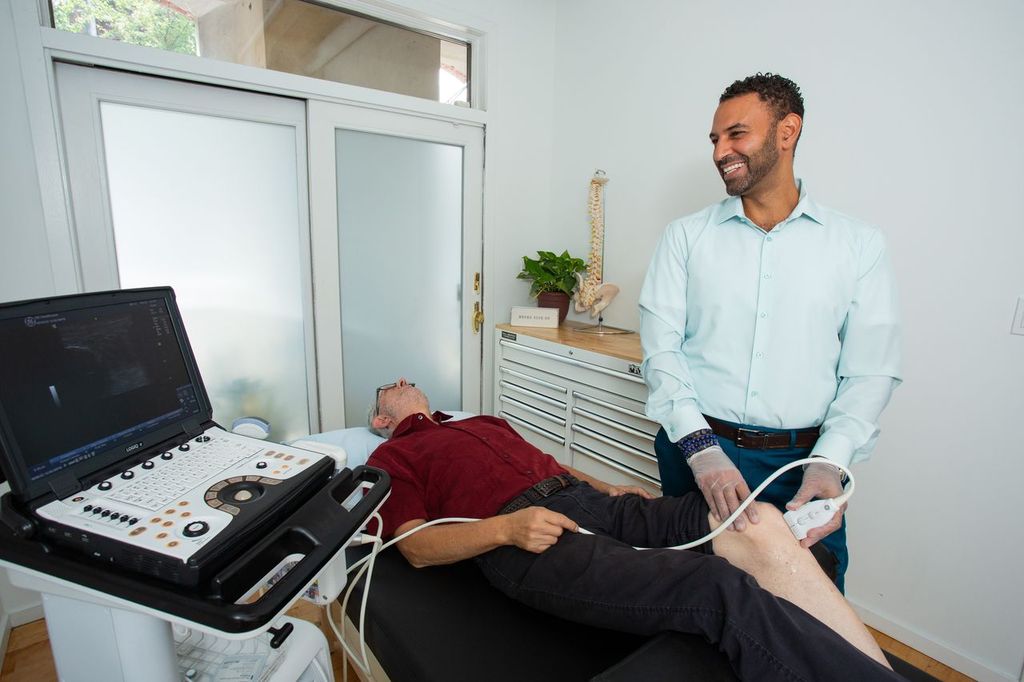
3. Is image-guidance used for the delivery?
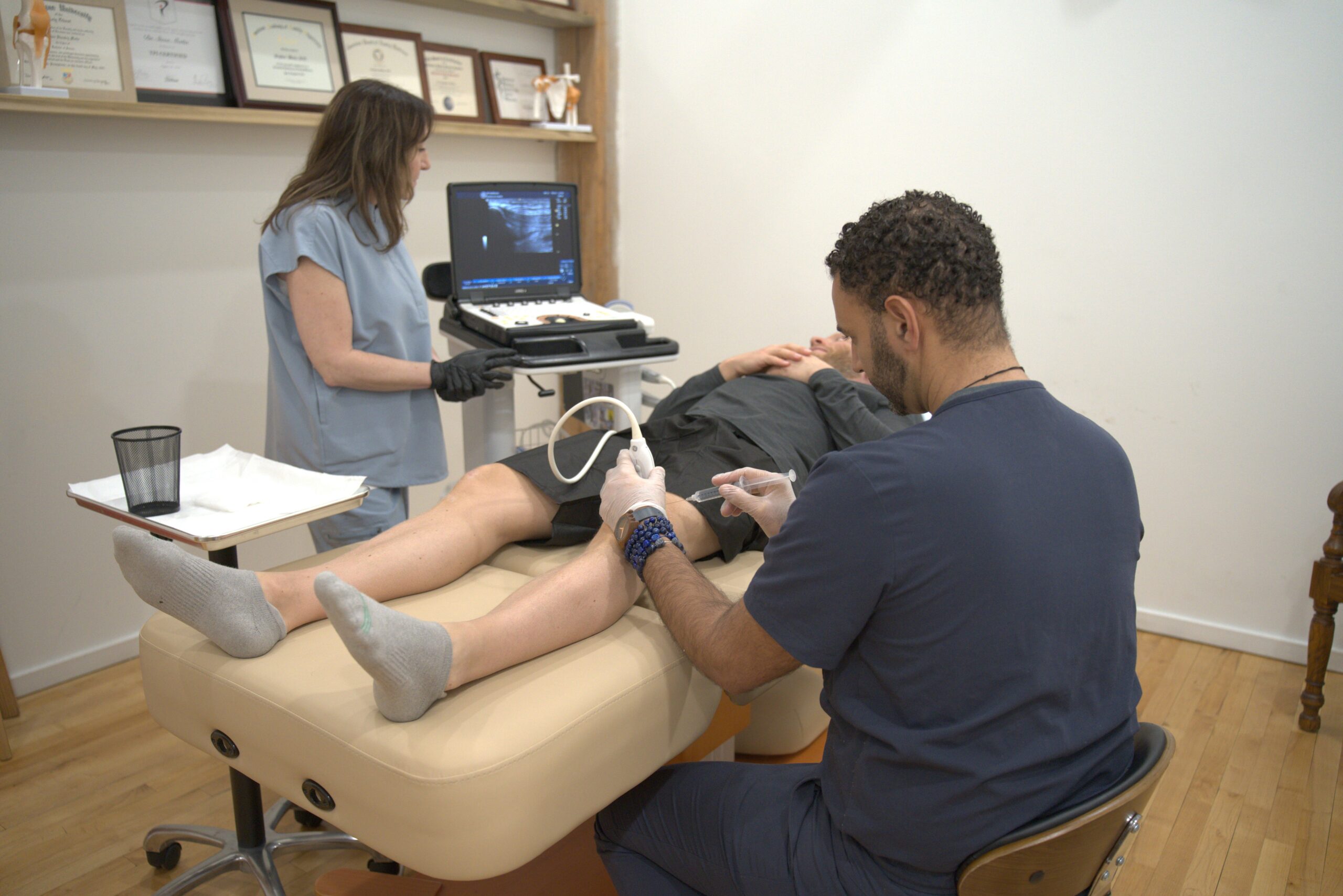
It absolutely should be! This is perhaps the most overlooked part of the process. Even the best cells in the world won’t work if they are injected into a fat pad instead of a torn ligament or an arthritic joint space.
- Why it Matters: “Blind” injections (relying on feel) have a high margin of error. Using Musculoskeletal Ultrasound allows the physician to see the needle enter the exact target area in real-time.
- The Standard: Precision is the difference between a failed procedure and a life-changing result. If a clinic doesn’t use a screen to guide the needle, the procedure is significantly less accurate.
4. What is the clinic’s stem cell storage and safety protocol?
A knowledgeable provider treats these cells with rigor and safety. How the cells were handled and stored is vital to their success.
- Maintaining Therapeutic Properties: Biological signals are fragile. Ask how the clinic manages storage; if they are not stored at precise temperatures, their regenerative potential can be compromised.
- Laboratory Selection: A reputable clinic should prioritize labs that use rigorous, third-party testing for sterility and endotoxins to ensure every injection is optimized for safety.
- Transparency: Reputable providers use products with a clear, documented history from donor screening to the moment of injection.
5. How do you optimize treatment outcomes?
Think of stem cells as seeds; they might not grow in dead soil. If a patient is highly inflamed, has uncontrolled blood sugar, or has significant hormonal deficiencies, the injected cells may die or fail to signal correctly.
- Why it Matters: A regenerative and functional medicine approach looks at the whole person. Optimization might include a pre-procedure anti-inflammatory diet, specific supplements, or peptide therapy (like BPC-157) to prime the area for healing.
- The Standard: Your clinic should discuss other aspects of your health and your current medications before scheduling an injection.
- The Red Flag: Avoid clinics that operate as injection mills, where you walk in, get a shot, and walk out without a discussion about your underlying health.

6. What does your follow-up and data collection look like?
Regenerative medicine is a journey, not a single event. The true work of tissue remodeling takes 3 to 6 months to reach its peak. Sometimes it requires more than one treatment.
- Why it Matters: A clinic should have a structured follow-up schedule (e.g., 1 week, 6 weeks, 3 months) to track your progress and adjust your protocol.
- The Standard: Ask the clinic about previous patient outcomes for your specific condition (e.g., arthritic joints vs. a meniscal tear). Even though each case is unique, they should be able to give you helpful information.
Making an Informed Choice
We understand that the path to recovery can be daunting. You deserve a provider who values your safety and your results as much as you do. If a clinic is hesitant to answer these six questions, they may not be the right fit for your regenerative journey.
Ready to find clarity in your recovery journey?
Don’t navigate the complexities of stem cell therapy alone. Experience the difference that triple board-certified expertise and precision-guided care can make. Book a discovery call today and find out if our advanced cellular protocols are the right fit for your goals.
Recommended Articles
- Intro to Stem Cell Therapy
- PRP vs. Stem Cell Therapy: What’s the Difference
- PRP vs. Stem Cell Therapy: Which Regenerative Treatment Is Right for Your Joint Pain?
- Stem Cell Injections for Shoulder Pain in Philadelphia: Heal Without Surgery
Written by Amanda Bates, RN and medically reviewed by Dr. Stephen Matta.